Engaging Undergraduates in Mechanisms of Tubular Reabsorption and Secretion in the Mammalian Kidney
Editor: Justin Shaffer
Published online:
Abstract
If students fail to see the connections among physiological systems, they can become overwhelmed with the amount of information they need to learn. Some students have particular difficulty with the renal system for this reason. This lesson was developed to emphasize two general models in physiology that can inform student understanding of tubular reabsorption and secretion. In this two-hour lesson, students learn the mechanisms of tubular reabsorption and secretion by drawing on their prior knowledge of transport across physiological membranes (general model 1). Students also apply their knowledge of the Starling forces of capillary exchange (representing general model 2) as they learn how tubular reabsorption is regulated. The lesson is a combination of mini-lectures, used to introduce learning outcomes and more specific information, and group active learning exercises that ask students to recall prior knowledge of the two general models in physiology, make predictions, and synthesize and organize their knowledge. This lesson has fit well in a structured, upper-division physiology course.
Primary image: Reabsorption and secretion in the renal tubule. Overview of the role of reabsorption and secretion in the formation of urine. Substances may be reabsorbed from tubular fluid or secreted into it to maintain homeostasis in body fluid volume and composition.
Citation
Roosa KA. 2021. Engaging undergraduates in mechanisms of tubular reabsorption and secretion in the mammalian kidney. CourseSource. https://doi.org/10.24918/cs.2021.4
Society Learning Goals
Cell Biology
- Membrane Structure and Function
- How do solutes and other materials move across membranes?
Lesson Learning Goals
- Students will understand the ways that reabsorption and secretion determine what is excreted by the kidney.
- Students will recognize how transport across membranes and mass flow relate to renal reabsorption and secretion.
From Human Anatomy and Physiology Society Learning Goals (https://www.hapsweb.org/page/learning_goals):
- Explain how body systems work together to maintain homeostasis.
- Identify anatomical structures and describe complex interrelationships between structure and function.
Lesson Learning Objectives
Students will be able to:
- Describe the process by which substances are reabsorbed or secreted in the nephron by passive diffusion, primary active transport, and secondary active transport.
- Explain what causes the transport maximum for certain substances in the renal tubule.
- Explain how water is reabsorbed in the renal tubule.
- Describe the characteristics of the different segments of the nephron. List, in general, what is reabsorbed/secreted by each.
- Describe mechanisms for reabsorption and secretion in a particular segment of the nephron given a figure.
- Predict how changes to the hydrostatic and colloid osmotic forces in the kidney will affect tubular reabsorption.
- Define the molecular function of aldosterone, angiotensin II, and anti-diuretic hormone on the renal tubule and the overall effect on water and sodium reabsorption.
Article Context
Course
Article Type
Course Level
Bloom's Cognitive Level
Vision and Change Core Concepts
Class Type
Class Size
Audience
Lesson Length
Pedagogical Approaches
Principles of How People Learn
Assessment Type
INTRODUCTION
Background Scientific Information
The kidneys have several important homeostatic functions. Among these are regulating body fluid balance and blood volume/pressure. Tubular reabsorption and secretion in the nephron allow for precise control of body fluid volume and composition. During reabsorption, water and/or solutes move from the renal tubule to the interstitium. From the interstitium they move into the peritubular capillaries surrounding the renal tubule. Water and solutes cross these barriers in the opposite direction during secretion.
The movement of water and solutes during reabsorption and secretion is governed by the processes of diffusion, osmosis, and active transport. Either an electrochemical gradient or ATP is necessary to drive these processes. The Na+/K+ ATPase is a primary source of ionic gradients across tubular cell membranes that drive the reabsorption and secretion of solutes and water by secondary active transport (1). Water moves by osmosis when the tubular wall is permeable to it and an osmotic gradient exists (2).
There are two major routes for the movement of water and solutes between the tubular fluid and the interstitium. When solutes/water cross the tubular cells through pumps, channels, or simple diffusion, they take the transcellular route. Alternatively, in some segments of the nephron, the paracellular pathway is significant, where solutes/water move between the interstitium and tubular fluid by traveling between the tight junctions that hold tubular cells together. The permeability of the tight junctions varies throughout the nephron, with higher permeability in the proximal tubule as compared to the rest (2). The reabsorption of water through the paracellular pathway may also move dissolved solutes along with it, known as solvent drag (1).
Structural and functional differences exist among the segments of the nephron that dictate which substances pass between the tubular fluid and the renal interstitium. For example, the proximal tubule is a site of significant reabsorption of water and solutes such as sodium, glucose, and amino acids. The tubular cells in this region are rich in transport proteins for the aforementioned solutes and have a high metabolic rate, and a microvilli brush border vastly increases the surface area for transport (2). The paracellular route of transport is significant here as the tight junctions are relatively more permeable to water and solutes in this segment (2).
The processes of reabsorption and secretion must be regulated to maintain homeostasis under changing conditions (e.g., dehydration vs. overhydration). The Starling forces govern the movement of fluid across any capillary membrane. They include the capillary hydrostatic pressure (Pc), the interstitial fluid hydrostatic pressure (Pif), the plasma colloid osmotic pressure (Πc), and the colloid osmotic pressure of the interstitial fluid (Πif). Capillary hydrostatic pressure and interstitial fluid colloid osmotic pressure both promote filtration, whereas interstitial fluid hydrostatic pressure and the plasma colloid osmotic pressure oppose filtration. This relationship can be summarized by the following equation (2):
NFP = Pc — Pif — Πc — Πif
Where NFP is the net filtration pressure. Filtration of fluid through a capillary wall is then summarized by this equation:
Fluid flow across cappillary wall = Kf × NFP
Where Kf is the filtration coefficient of the capillaries. The filtration coefficient takes into account the permeability of the capillaries and their density in the capillary bed. When NFP is positive, fluid will be filtered from the capillary to the interstitium. When NFP is negative, fluid will be reabsorbed from the interstitium to the capillary (2).
The peritubular capillaries are unique in that the NFP is normally negative as compared to other "typical" capillaries in the body, promoting capillary reabsorption. Because they sequentially follow the glomerular capillaries where large amounts of fluid move from the capillary to the Bowman's capsule, Πc is relatively high. The volume of blood flow, and in effect the Pc, in the peritubular capillary is regulated by the rate of blood flow through the glomerulus, which is guarded by the efferent arteriole. In addition, the peritubular capillaries have a relatively high filtration coefficient, due to their large surface area in the renal tissue and their high fluid conductance (3). In this case, the high filtration coefficient promotes large amounts of reabsorption because the balance of the Starling forces yields a negative NFP.
While the conditions of the peritubular capillary are unique in that reabsorption is favored, consideration of the Starling forces provides a basis for understanding how tubular reabsorption is regulated in the face of blood pressure and body fluid changes. Any increase in Pc of the peritubular capillary decreases the amount of fluid reabsorbed by the nephron, thereby increasing the volume of urine produced. This could be the result of an overall increase in arterial pressure or a decrease in resistance of the efferent arteriole, which causes a relative increase in blood flow and Pc in the peritubular capillary. Conversely, any decrease in Pc will increase the volume of water reabsorbed by the peritubular capillaries and decrease urine output. This could be the result of reduced arterial pressure or increased resistance of the efferent arteriole and the corresponding decrease in blood flow through the peritubular capillary.
Tubular reabsorption is also regulated by hormones. The actions and stimuli for these hormones are summarized in Table 1. Angiotensin II (AngII) has effects on both the Starling forces and transcellular transport in the tubular cells. By constricting the efferent arteriole of the glomerulus, it increases peritubular capillary reabsorption by both increasing the colloid osmotic pressure and decreasing the hydrostatic pressure of the peritubular capillary. Angiotensin II also increases the transport of Na+ across tubular cells into the renal interstitium, which is followed by water (2). Aldosterone, which is secreted by the adrenal cortex in response to elevated AngII, increases sodium reabsorption by the cortical collecting tubule. It stimulates the synthesis of the Na+/K+ ATPase on the basolateral membrane of the tubular cells. At the same time, it stimulates the production of Na+ and K+ channels on the luminal membrane (2). The additional removal of Na+ from the basolateral side of the cell creates a stronger gradient for the ion to move from the tubular lumen across the cell through the new luminal sodium channels. Anti-diuretic hormone (ADH) increases the permeability of the distal tubule, collecting tubule, and collecting duct to water, promoting its reabsorption.
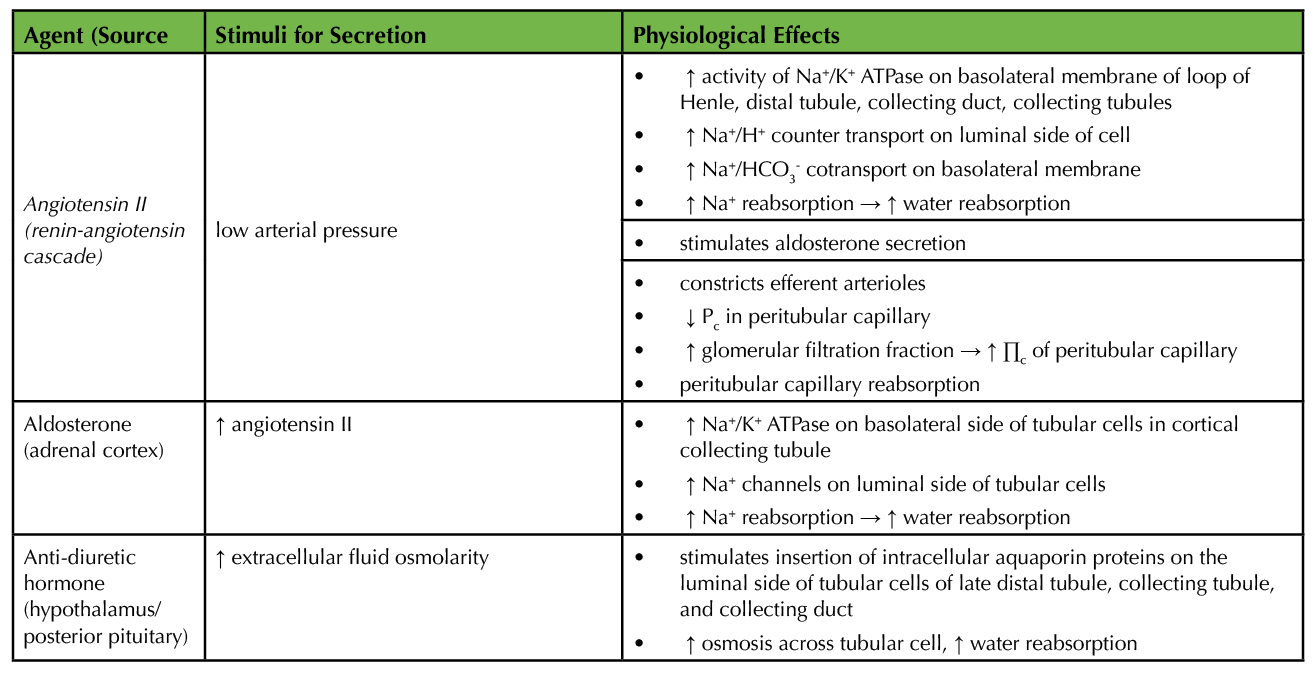
Table 1. Summary of hormonal regulation of tubular reabsorption (2).
Rationale for Lesson Format
One of the difficulties students may have in learning physiology is that as body systems are introduced, they may view concepts within each system as discrete and fail to make connections between them. Students often feel that they need to learn each new system from scratch and can be overwhelmed by the volume of information. In reality, many of the concepts in seemingly disparate situations are rooted in the same general physiological principles. The Human Anatomy and Physiology society has highlighted the need for students to be able to "Recognize and apply patterns that unify, organize, and simplify the abundant detail of anatomy and physiology" as one of their learning goals for undergraduate students (https://www.hapsweb.org/page/learning_goals.). The act of transfer, taking knowledge from one area and using it in a new situation, can be difficult for students in physiology (4). Emphasizing general models in physiology is an approach to help students see common underlying general principles and transfer them as they encounter new physiological systems (5,6). For example, the topics of both vascular and renal physiology both rely on concepts of fluid dynamics. If students have a good understanding of fluid dynamics in general, they can transfer that knowledge between the vascular and renal systems. Helping students recognize the general physiological models may help them learn complex concepts more easily and reduce the burden of detail.
Renal physiology, particularly ion and fluid dynamics in the nephron, are difficult concepts for physiology students to learn (7-9). Students may miss the relation to their prior knowledge of transport across membranes and fluid dynamics. This lesson introduces students to the mechanisms of renal tubule reabsorption and secretion and their regulation. The lesson described here uses two general models to that are common among physiological systems: 1) transport across membranes, which includes diffusion, osmosis, and carrier-mediated transport, and 2) mass and heat flow, which involves relationships between pressure and flow and diffusion, osmosis, and ion flow (5). The lesson guides students as they transfer their prior knowledge of these general physiological models to renal reabsorption and secretion.
The lesson was designed for an upper-division, lecture-only undergraduate course that is supported by the first half of Guyton and Hall's Textbook of Medical Physiology (2). The lesson corresponds to Renal Tubular Reabsorption and Secretion (chapter 28) in Guyton and Hall. Any anatomy and physiology text used to teach two-semester anatomy and physiology courses would also be an appropriate support material for this lesson, for example, Openstax Anatomy and Physiology (10) or Marieb and Hoehn's Anatomy and Physiology (11). It is part of a structured physiology course that features regular in-class active learning exercises, weekly homework assignments, and several mid-term exams. Table 2 provides an outline of how the learning objectives of the lesson align with society and learning framework goals.
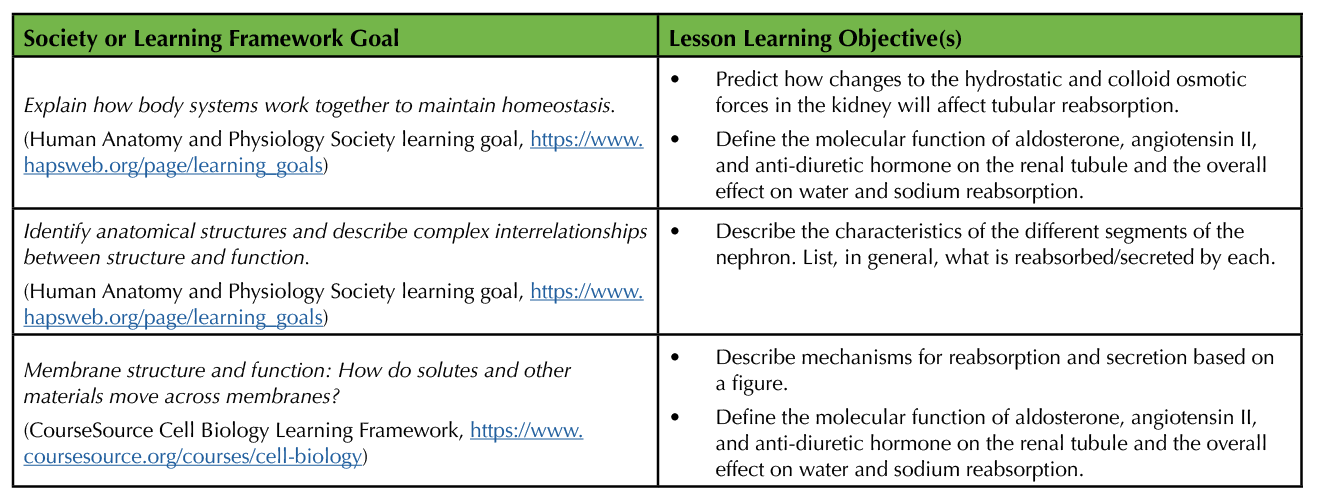
Table 2. Alignment of lesson learning objectives with society and learning framework goals. From Human Anatomy and Physiology Society learning goals (https://www.hapsweb.org/page/learning_goals) and Cell Biology Learning Framework (https://www.coursesource.org/courses/cell-biology).
Over the course of two 50-60-minute class periods, brief lectures to introduce topics are combined with activities that allow students to draw on their prior knowledge of the general physiological models to build an understanding of tubular function. The format of the two-hour lesson is based on findings that indicate students in biology tend to prefer classes that combine lecture with active learning exercises rather than classes devoted to 100% active learning exercises (12). Accordingly, the two sessions in this lesson are split between brief lectures, activities completed in small groups, and whole-class discussion. Furthermore, the activities are designed to allow students to practice the skills of making predictions and organizing new information.
In the first class session, students are introduced to the basic concepts of tubular reabsorption and secretion. Students use their prior knowledge of diffusion, osmosis, and active transport (the transport across membranes general model) as they learn the cellular mechanisms of reabsorption and secretion throughout the segments of the nephron. They also build on their understanding of the role of the Na+/K+ ATPase in cellular transport. Students organize their new knowledge in a summary table.
The second session is focused on the mechanisms that regulate tubular reabsorption. Students complete an activity that requires them to apply their prior knowledge on the impact of Starling forces (the mass and heat flow general model) on capillary reabsorption to the peritubular capillary. They derive the reasons that elevated arterial pressure is associated with increased urine output. Once this new knowledge is established, students build on it further to better understand the ways that hormones (aldosterone, angiotensin II, etc.) regulate tubular reabsorption by influencing the Starling forces and transport across the tubular membrane on the cellular level.
Intended Audience
Advanced (3rd/4th year) undergraduate biology majors in human/mammalian physiology.
Required Learning Time
Two 50 to 60-minute class periods.
Prerequisite Student Knowledge
Students should have prior knowledge of the mechanisms of transport across a membrane, including diffusion, osmosis, and primary and secondary active transport. They should be able to interpret a diagram depicting each of these processes and make predictions about the movement of solutes and water based on an electrochemical gradient.
Students should be able to define the four Starling forces of capillary exchange (capillary hydrostatic pressure, interstitial fluid hydrostatic pressure, plasma colloid osmotic pressure, and interstitial fluid colloid osmotic pressure). They should be able to interpret the effect of changes to vascular resistance/pressure and plasma protein concentration on the forces. They should be able to explain how each of the forces contributes to filtration and reabsorption in a capillary. Given values for hydrostatic and colloid osmotic pressure, students should be able to calculate the net force for fluid movement.
Prerequisite Teacher Knowledge
In addition to the prerequisite knowledge required for students, the teacher should be able to describe the processes of tubular reabsorption and secretion and explain how these processes contribute to the formation of urine. The instructor should be able to explain why the Na+/K+ ATPase is important for generating electrochemical gradients that drive reabsorption and secretion throughout the nephron. The teacher should be able to relate the Starling forces for capillary exchange to reabsorption by the peritubular capillary and outline the mechanisms of action of anti-diuretic hormone, aldosterone, and angiotensin II (Table 1).
Appropriate support materials for this lesson include Guyton and Hall's Textbook of Medical Physiology (chapters 16 and 28; 2), Medical Physiology: A Cellular and Molecular Approach (chapters 20 and 35; 3), Principles of Renal Physiology (chapters 4-6 and 13; 1).
SCIENTIFIC TEACHING THEMES
Active Learning
Brief lectures are integrated with in-class small group (2-3 students) worksheet activities. The activities ask students to gather, organize and summarize information, make predictions, and form explanations for physiological phenomena.
Assessment
Learning was first formally assessed on a low-stakes homework assignment, which students could use their notes to answer. Questions related to this lesson were also on the third mid-term exam and final exam.
Inclusive Teaching
This lesson is highly structured and involves active learning, which promotes participation by more students, including underrepresented minorities and first-generation students (13,14). Students are given quiet time to work on the problems before each class discussion, which invites more students to form thoughts and participate (15). Since there are multiple opportunities for groups to participate in the class discussion, the instructor can devise a way to hear from all/most groups (for example, assign specific groups to respond to each question in the exercises). Students work in small groups of 2-3. The instructor may also form the work groups to increase the mixing of students outside their typical social circles.
LESSON PLAN
This lesson is split into two 50 to 60-minute sessions. The activities for each session are outlined in Table 3.
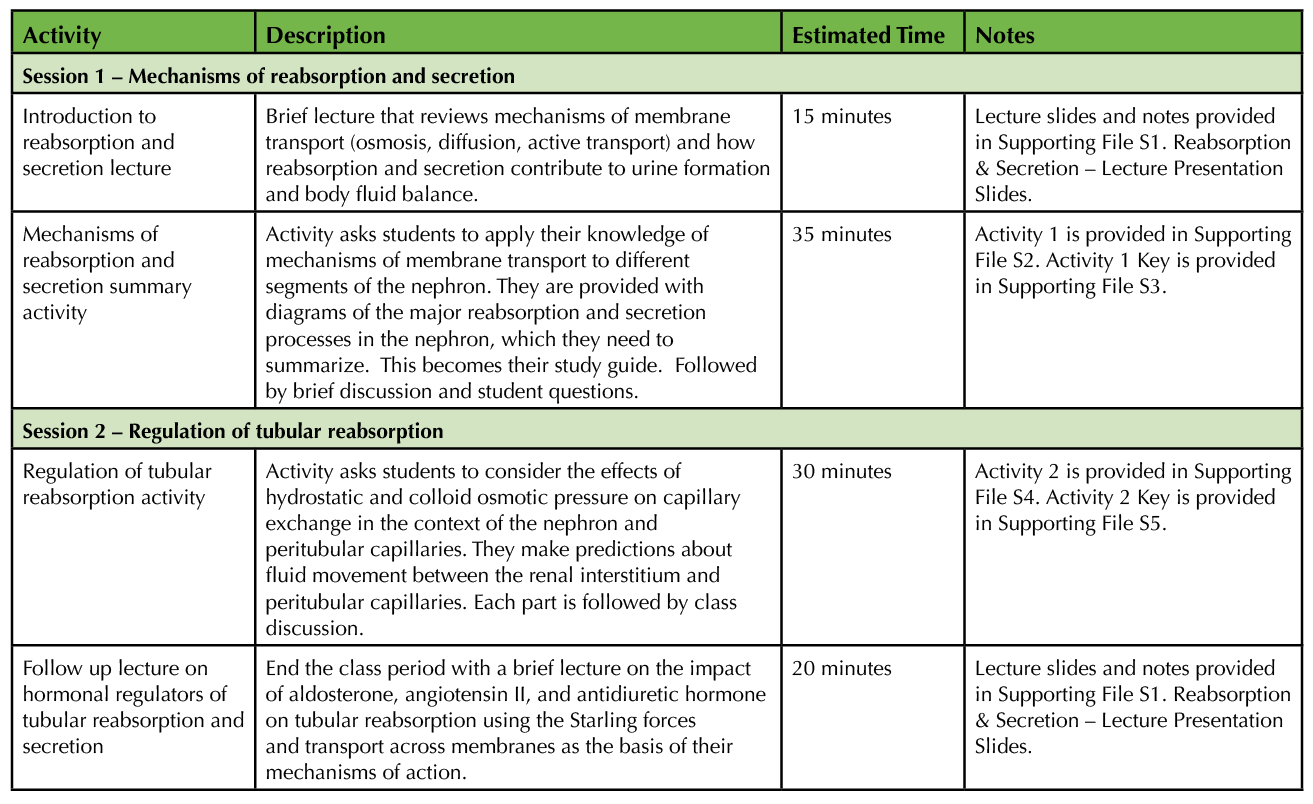
Table 3. Outline and timetable for lesson activities.
Session 1
Begin by introducing the learning outcomes and then give a brief introduction (about 15 minutes) to the basics of reabsorption and secretion, according to the outline below (see Supporting File S1. Reabsorption & Secretion – Lecture Presentation Slides for figures and lecture notes).
1. Define reabsorption and secretion in the renal tubule (i.e., reabsorption is the movement of water and solutes from tubular fluid to blood and secretion from blood to renal tubular fluid).
2. For any substance in the blood, excretion = filtration – reabsorption + secretion.
3. Overview of the mechanisms by which substances move between the renal tubule, renal interstitium, and peritubular capillaries (i.e., review mechanisms by which substances cross cell membranes).
- Water or solutes travel on the paracellular pathway to cross between the blood and tubular fluid. They move between renal tubule cells and travel through the tight junctions that hold them together.
- Or, water and solutes travel on the transcellular pathway where they cross the tubular cells to move between the blood and tubular fluid
- Simple diffusion: requires electrochemical gradient and permeability.
- Active transport: requires a pump (and energy) to move substances across the membrane.
- Secondary active transport: An electrochemical gradient set up by a pump drives the diffusion of another substance.
- Stress the importance of the Na+/K+ ATPase in setting up gradients for secondary active transport.
4. Discuss the structural differences in the tubular cells throughout the nephron (e.g., the transporters expressed in the proximal tubule differ from those in the collecting duct, where there is a brush border present, etc.) and how the structure relates to functional differences.
5. Discuss the concept of transport maximum using glucose reabsorption in the proximal tubule as an example.
After the introductory lecture, students complete the first in-class activity (Supporting File S2. Reabsorption & Secretion – Activity 1) in small groups (2-3 students). This activity is a table to guide students as they gather and summarize information on which substances are reabsorbed and secreted throughout the nephron and the mechanisms for each. Rather than requiring students to memorize all substances reabsorbed and secreted in each segment of the nephron and the cellular mechanism for each substance reabsorbed or secreted, I focus on their ability to interpret a figure of the renal tubule that depicts a mechanism of reabsorption or secretion across the tubular cell. I also expect them to have a general idea of what is exchanged at each segment. For example, they should know that amino acid and glucose reabsorption occur in the proximal tubule and that the collecting duct reabsorbs water. Given a figure similar to what is provided in the table, they should be able to explain the mechanisms for glucose and amino acid reabsorption in their own words.
The table includes diagrams depicting each segment of the nephron. For each diagram students should describe the mechanisms for transport in one column, then make a summary of which substances are reabsorbed or secreted in the next column. It is helpful to complete the first row of the table (proximal tubule) as a class, modeling the type of information you think is important to summarize. It is also an opportunity to stress again how important the Na+/K+ ATPase is in the movement of solutes across the tubular wall. After the students complete the table, the diagrams are reviewed as a class (using images in Supporting File S1. Reabsorption & Secretion – Lecture Presentation Slides), and we discuss what they filled into their tables. A key to this activity is provided in Supporting File S3. Reabsorption & Secretion – Activity 1 Key. The session ends with a wrap-up, reviewing the importance of the Na+/K+ ATPase in tubular transport, and a preview of the second hour in which students will learn how tubular reabsorption is regulated.
This lesson was used in a 50-minute class period. To adapt session 1 for a 60-minute class period, the instructor may consider adding a brief low-stakes review quiz or clicker questions between the lecture and the first activity or after completing the activity.
Session 2
The second part of this lesson covers how tubular reabsorption is regulated. We begin with an introduction to the learning objectives. Students then complete an activity that asks them to apply their prior knowledge of the Starling forces of capillaries to the renal interstitium and peritubular capillaries (Supporting File S4. Reabsorption & Secretion – Activity 2), which requires about 30 minutes. The overall goals of the activity are to predict how changes to hydrostatic and colloid osmotic pressures influence peritubular reabsorption and to derive an explanation for greater urine output during elevated blood pressure. The activity occurs in three parts.
Part I asks students to calculate the net force and direction for fluid movement between the peritubular capillaries and renal interstitium given a diagram with values for Pc, Pif, Πc, and Πif. They determine that the conditions given in the activity yield a net pressure that promotes reabsorption in the peritubular capillary. They then devise ways that tubular reabsorption could be increased or decreased by changing either the hydrostatic pressure or colloid osmotic pressure of the system. This is intended for practice with the relationship between the Starling forces and capillary reabsorption in the new context of tubular reabsorption. Part I of the activity is wrapped up with a brief review of student responses and by addressing any misconceptions before taking the concepts any further. Supporting File S1. Reabsorption & Secretion – Lecture Presentation Slides provides images and additional notes to aid in discussion. Upon wrap up, I stress that students already knew how to answer questions like these since we had already covered these concepts in the unit on the cardiovascular system. They are simply applying this prior knowledge to the renal system.
In part II of the activity, students make predictions about the impact of changes to vascular pressure and colloid osmotic pressure on peritubular reabsorption. After completing the two tables in part II, there is again a discussion of student responses. Students tend to have the most difficulty predicting the impact of "greater fraction of plasma filtered in the glomerulus" on peritubular colloid osmotic pressure and peritubular reabsorption. Some time is usually spent reviewing how glomerular filtration generally excludes proteins and how a higher rate of glomerular filtration will increase the colloid osmotic pressure of the plasma exiting the glomerulus and entering the peritubular capillaries.
In part III students apply the concepts covered in parts I and II to explain why increased arterial pressure leads to increased urine production. For the remainder of the class (about 20 minutes), there is a brief lecture on the impact of hormones on tubular reabsorption, calling on their mechanisms as they relate to the Starling forces and transport across cell membranes. Any additional time in a 60-minute class period could be used for review/clicker questions between parts of the activity.
Lecture outline
Stimuli, mechanisms, and overall effects of the following on tubular reabsorption (as reviewed in Table 1, see Supporting File S1. Reabsorption & Secretion – Lecture Presentation Slides for figures and lecture notes):
- Aldosterone
- Angiotensin II
- Antidiuretic hormone
The hormonal effects on the renal tubule tend to be the most difficult parts of this lesson for students to learn. In the lecture, if time permits, I show students the diagram of each hormone mechanism on the tubular cell and ask them to take a minute or two to jot down what they see happening in the figure. We then go over each as a group. This step may help students recognize the usefulness of their prior knowledge instead of jumping right into a lecture, which might imply that it is all new information.
TEACHING DISCUSSION
Renal physiology incorporates several general physiological models (5). The processes of reabsorption and secretion can be learned as students build on their general understanding of transport across membranes and mass flow. This interactive lesson allows students to construct and organize new knowledge on the mechanisms of tubular reabsorption and secretion and their regulation.
Student Participation and Performance
In an upper-division physiology class of 30 students, this lesson stimulated nearly 100% participation. Lessons with this structure, based on other published teaching resources, are a regular feature of this course. The unit on renal physiology was near the end of the term when students were in a routine of the mini-lecture/activity format, which likely influenced participation. Interestingly, the first time using this lesson, with a class of only 12 students, a small proportion of the class was resistant to participate. Students often become accustomed to the passive, didactic classroom, and many are resistant to deviations from the traditional lecture format (16). These students are accustomed to receiving unambiguous facts from the instructor in their other courses and taking those facts home to learn (12). I have observed students who are reluctant to write responses on their papers until validated by the instructor. A thorough introduction to the philosophy and value of active learning early in the term is important for generating student buy-in, and this was done at every opportunity in the larger, 30-student class. Students should be reminded that their participation, taking risks, and the process is the important part of the exercise when it comes to learning rather than having the right answer immediately. I emphasize this regularly at the start of the term and provide opportunities to meet student needs for a clean paper with the right answers on it. For example, I encourage the use of pencils over permanent ink and provide downloads of activities after class for those who want a clean copy for their notebooks. The incorporation of mini-lectures with the student-centered exercises also likely reduces barriers to participation, as they may satisfy student needs to have facts delivered by the instructor (12). In course evaluations students have noted that in-class activities, such as those in this lesson, were helpful and that they appreciated the regular opportunities to work with the material.
Student learning was assessed one week after the lesson with a homework assignment that included typical test questions. The percent of the class that responded correctly to homework items pertaining to the lesson is shown in Table 4. Over 80% of students responded correctly to questions that asked them to describe the effects of ADH on the renal tubule, predict how changes to the Starling forces affect peritubular reabsorption, and explain how resistance of the afferent arteriole affects hydrostatic and colloid osmotic pressure. Students had the most difficulty when they were asked to use these same concepts and essentially work backward, choosing a reason that peritubular capillary reabsorption would be decreased. Only 53.6% of students responded correctly to this question. More practice with this skill could be added to the end of activity 2 with sample questions.
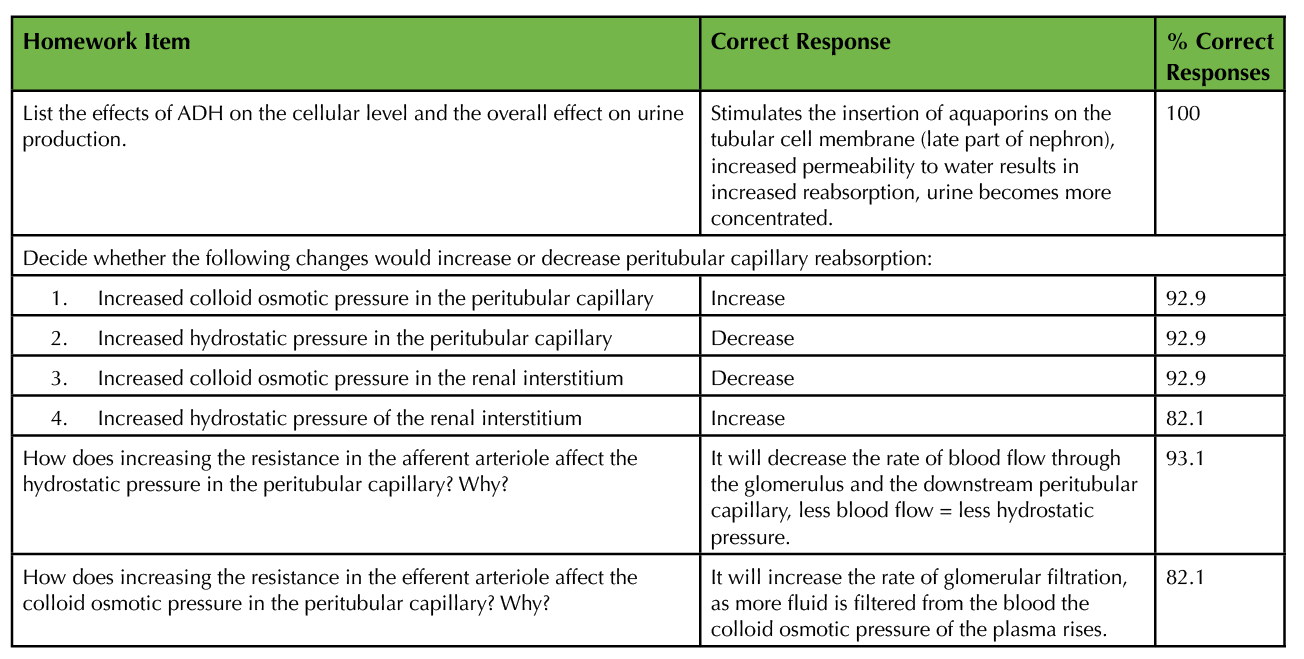
Table 4. Student achievement on homework items assessing learning associated with this lesson. Sample size was 28 students.
Possible Modifications
While there are opportunities for students to answer questions and receive feedback from the instructor throughout the exercises, this lesson could be improved by adding more opportunities for students to reflect on their learning and check their understanding with test-like questions. Placing typical test questions between the lecture and activity blocks in the lesson may also help both students and the instructor assess whether the class is ready to move on to the next concept or if further discussion is needed. These could be completed in a think-pair-share format to promote discussion and participation by all students.
This lesson could be adapted for asynchronous online instruction. Table 5 provides a sample lesson structure. The mini-lectures could be replaced with videos, each followed by a brief formative assessment (e.g., multiple-choice quiz). Students could be asked to complete activities 1 and 2 synchronously in small groups, if technology allows (i.e., breakout rooms on a videoconferencing platform), with whole class discussion between each part. In an asynchronous environment, students would complete part of the exercise and then watch a brief video that explains the important concepts after the student submits their responses (i.e., adaptive release of videos after submission of the assignment). This would be repeated after each part of the exercise.
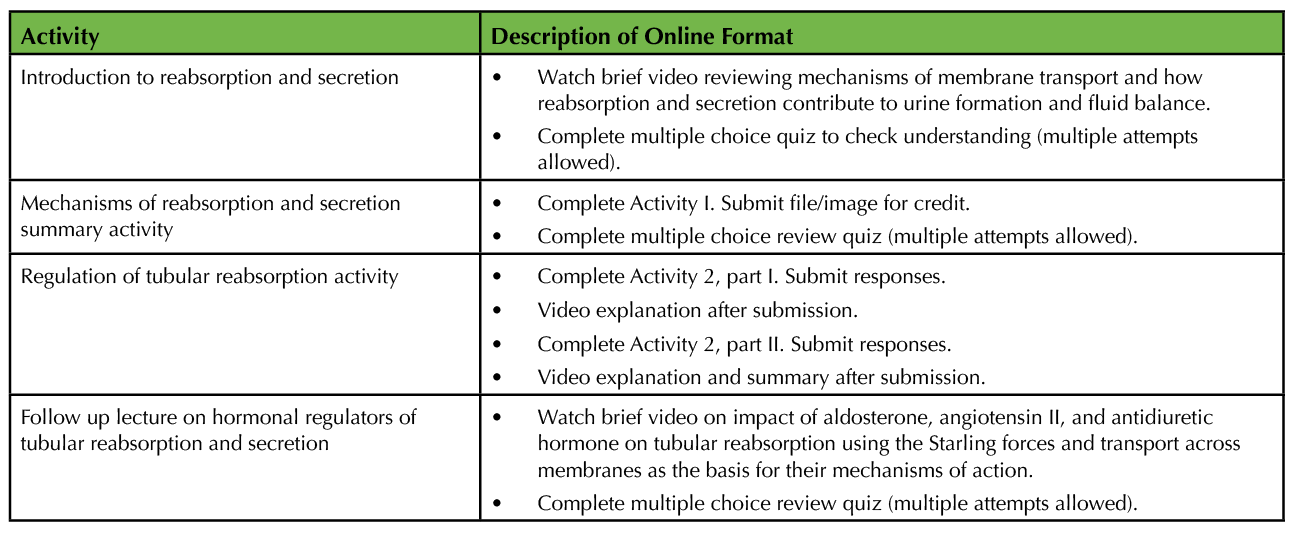

Table 5. Sample online format of lesson.
The lesson could be successfully used in larger physiology courses. All activities would be conducted in the same way in small groups of 2-3 students. A teaching assistant would be helpful for monitoring group progress and answering questions during the activities. To get a better picture of how students are doing with each activity, a student response system could be used for formative assessment at stopping points during the lesson (e.g., after mini-lectures or between parts of each activity). The instructor could either use questions from the activity (converted to multiple choice) or more general review questions for the student response system.
This lesson could be adapted for two-semester human anatomy and physiology courses. The mini lectures and activity on summarizing the substances and mechanisms reabsorbed and secreted throughout the nephron would be useful in this context. The first activity provides students with both a review of mechanisms of transport across membranes and new information on tubular transport. The second activity on regulating reabsorption and secretion through the Starling forces may need to be eliminated or significantly modified to fit this type of course, depending on the instructor's goals. In allied health courses, the action of diuretics could be added to the discussion of mechanisms of reabsorption and secretion in session 1 (e.g., thiazides) as well as the discussion of hormones that regulate reabsorption in session 2 (e.g., spironolactone).
This lesson could be built upon to develop a highly student-centered unit on renal physiology. The Starling forces provide a basis for understanding glomerular filtration, and activities similar to activity 2 (Supporting File S4. Reabsorption & Secretion – Activity 2) could be developed for the topic. Students could predict how changes to afferent and efferent arteriole resistance impact hydrostatic and colloid osmotic pressure, and as a result, further glomerular filtration. The lesson presented here could be incorporated with Braga's activity on tubular reabsorption where students interpret data on glucose transport to understand transport saturation in the renal tubule (17). This may be useful for more junior students studying renal physiology.
SUPPORTING MATERIALS
- S1. Reabsorption & Secretion – Lecture Presentation Slides. S1 includes images and notes for both brief lectures and images from activities for post-activity discussion.
- S2. Reabsorption & Secretion – Activity 1
- S3. Reabsorption & Secretion – Activity 1 Key
- S4. Reabsorption & Secretion – Activity 2
- S5. Reabsorption & Secretion – Activity 2 Key
ACKNOWLEDGMENTS
I thank the students of Mammalian Physiology I at SUNY Oneonta for their participation in this lesson and Ed Beck for his review of this lesson. I am also grateful to two anonymous reviewers for their critical review and comments on an earlier draft. Data collection on student performance was approved by the Institutional Review Board at SUNY Oneonta (Study # 2495).
References
- Lote CJ. 2012. Principles of Renal Physiology. 5th ed. New York, NY: Springer.
- Hall JE. 2016. Guyton and Hall Textbook of Medical Physiology. 13th ed. Philadelphia, PA: Elsevier.
- Boron WF, Boulpaep EL. 2012. Medical Physiology: A Cellular and Molecular Approach. 2nd ed. Philadelpha, PA: Saunders Elsevier.
- Goodman BE, Barker MK, Cooke JE. 2018. Best practices in active and student-centered learning in physiology classes. Adv. Physiol. Educ. 42(3):417-423. doi:10.1152/advan.00064.2018.
- Modell HI. 2000. How to help students understand physiology? Emphasize general models. Adv. Physiol. Educ. 23(1):101-7. doi: 10.1152/advances.2000.23.1.s101.
- Goodman BE. 2001. Pulmonary and renal pressure-flow relationships: what should be taught? Adv Physiol. Educ. 25(2):15-28. doi: 10.1152/advances.2001.25.2.15.
- Richardson D, Speck D. 2004. Addressing students' misconceptions of renal clearance. Adv. Physiol. Educ. 28:210-212. doi: 10.1152/advan.00021.2004.
- Tufts MA, Higgins-Opitz SB. 2009. What makes the learning of physiology in a PBL medical curriculum challenging? Student perceptions. Adv. Physiol. Educ. 33(3):187-95. doi: 10.1152/advan.90214.2008.
- Cheng HM, Durairajanayagam D. 2012. Misconceptions highlighted among medical students in the annual International Intermedical School Physiology Quiz. Adv. Physiol. Educ. 36(3):229-32. doi:10.1152/advan.00089.2011.
- Betts JG, Young KA, Wise JA, Johnson E, Poe B, Kruse DH, Korol O, Johnson JE, Womble M, DeSaix P. 2013. Anatomy and Physiology. Houston, TX: OpenStax.
- Marieb EN, Hoehn KN. 2019. Anatomy and Physiology. 7th ed. New York, NY: Pearson.
- Walker JD, Cotner SH, Baepler PM, Decker MD. 2008. A delicate balance: integrating active learning into a large lecture course. CBE Life Sci. Educ. 7(4): 361-7. doi:10.1187/cbe.08-02-0004.
- Eddy SL, Hogan KA. 2014. Getting under the hood: how and for whom does increasing course structure work? CBE Life Sci. Educ. 2014. 13(3): 453-68. doi:10.1187/cbe.14-03-0050.
- Haak DC, HilleRisLambers J, Pitre E, Freeman S. 2011. Increased structure and active learning reduce the achievement gap in introductory biology. Science. 332(6034): 1213-6. doi: 10.1126/science.1204820.
- Tanner KD. 2013. Structure matters: Twenty-one teaching strategies to promote student engagement and cultivate classroom equity. CBE Life Sci. Educ. 12:1-10. doi:10.1187%2Fcbe.13-06-0115.
- Luscombe C, Montgomery J. 2016. Exploring medical student learning in the large group teaching environment: examining current practice to inform curricular development. BMC Med. Educ. 16:184. doi: 10.1186/s12909-016-0698-x.
- Braga VA. 2011. Teaching the renal tubular reabsorption of glucose using two classic papers by Shannon et al. Adv. Physiol. Educ. 35(2): 114-6. doi: 10.1152/advan.00108.2010.
Article Files
Login to access supporting documents
Engaging Undergraduates in Mechanisms of Tubular Reabsorption and Secretion in the Mammalian Kidney(PDF | 191 KB)
S1. Reabsorption and Secretion - Lecture presentation slides.pptx(PPTX | 10 MB)
S2. Reabsorption and Secretion - Activity 1.docx(DOCX | 178 KB)
S3. Reabsorption and Secretion - Activity 1 Key.docx(DOCX | 181 KB)
S4. Reabsorption and Secretion - Activity 2.docx(DOCX | 74 KB)
S5. Reabsorption and Secretion - Activity 2 Key.docx(DOCX | 75 KB)
- License terms

Comments
Comments
There are no comments on this resource.